Pharmacists Integral to Continuity of Care at Scott and White Memorial Hospital
Work to Create High-Risk Medication Team Pays Off for Patients
DISCHARGE FROM HOSPITAL TO HOME or a long-term care facility is a busy time for both patients and care providers. When administrators at Scott and White Memorial Hospital, a 600-bed academic medical center in Temple, Tex., found that the computer-assisted discharge medication reconciliation process wasn’t robust enough, they tapped pharmacy staff for a solution.
Seizing the opportunity to demonstrate leadership, the pharmacy staff devised a plan, and with the hospital administration’s approval, the High-Risk Medication Team (HRMT) was born. Their endeavor successfully implements ASHP’s Pharmacy Practice Model Initiative recommendation for pharmacist involvement in establishing processes to ensure medication-related continuity of care.
Getting Off to a Good Start
Seeking to expand pharmacist duties often requires making a case to management, but at Scott and White, the administration had full faith in pharmacy staff from the start.

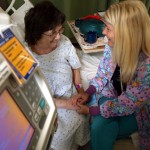
From left, Kurt Bradley Anderson, Pharm.D., staff pharmacist, consults with patient care pharmacists Lori Jackson-Khalil, Pharm.D., and Qing Xu, Pharm.D.
“We were fortunate that our leadership was in tune to this vulnerable period for patients,” said Tricia A. Meyer, M.S., Pharm.D., FASHP, of the HRMT. “They saw this as an opportunity for pharmacists based on our understanding of patient medication profiles and discharge medications.”
Tasked with providing options to the administration, the pharmacy staff set about devising several plans from which to choose. They met with the hospitalist, nursing staff, and leaders from different units to get their input and learn about their discharge processes.
Team members also called other institutions where they knew pharmacists had responsibilities similar to those they were seeking to obtain.
“We decided it would be a great opportunity for a new group of pharmacists to focus strictly on discharge,” said Meyer. “We already have pharmacists who focus on patient care, but they don’t have the time to dedicate to discharge.”
The team came up with three potential plans: One would cover medication review for every discharge; one would focus on high-risk patients and medications; and one would focus solely on anticoagulation. Administration opted for the second program, which focuses on high-risk.
From there, Meyer searched for a pharmacist who had expertise in patient interaction and counseling, and two additional team members who were ambulatory care specialists comfortable with counseling patients and reviewing medication profiles.
Working Past the Challenges
Although the pharmacy team did not have to worry about administrative buy-in, implementing the HRMT program was not without its challenges.
“One of the initial barriers we had was easily knowing when patients were to be discharged,” Meyer said. “Sometimes even the attending physician doesn’t know when the patient will be discharged. Test results or a change in the patient’s condition can extend or shorten a stay, and the physician might not know until rounds.”
The team tapped into several resources around the hospital, consulted with inpatient pharmacists, and accessed data from outpatient clinics, according to Lori Jackson-Khalil, Pharm.D., patient care specialist. “For example, the anticoagulation clinic has a list of patients, and we review that list each day. The cath lab would send us a list of patients on their schedule every day, as well.”
At first, software presented a challenge, said Jackson-Khalil. “We started with a spreadsheet in Excel, and we would manually input patient data. The trick was to set up the spreadsheet to give us the information we needed.”
The team decided to err on the side of caution and create detailed records.
“We kept data on everything—every visit to a patient’s room, every call to a physician, all categorized by drug and service. The team spent a lot of time documenting,” said Meyer. “But it was worth it. In the first six months or year of a new program, you are vulnerable. You have to show that you are accomplishing the goals the administration has given you. You can never keep too much data when trying to justify a program and its growth.”
Laborious data entry may soon be a thing of the past, however. The hospital is currently switching over to a new system that the staff believes will make it easier to identify which patients are about to be discharged.
Expanding Responsibilities
Once patients on high-risk medications are identified as transitioning to discharge, their orders are scanned to the pharmacy. Initially, the HRMT would review the orders and consult with prescribers as necessary regarding additions, possible errors in omissions, and unsafe prescribing conditions.
But as of November 2012, pharmacists are able to add medications or modify discharge orders. Their new responsibilities came about in part because they were able to demonstrate their impact on patient care through the data in their spreadsheets. For example, between January and June 2011, the team identified and successfully intervened in 42 unintentional omissions of high-risk medications such as phenytoin, warfarin, clopidogrel, and prasugrel.
“Now the administration sees us as a very effective team, and physicians call us and request that we add drugs to our oversight list,” said Meyer.
Pharmacy leadership in medication-related continuity of care is currently expanding. The team has begun counseling and oversight for patients with congestive heart failure in the hope that pharmacist-provided medication management at discharge will decrease readmissions.








 If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article.
If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article. Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore.
Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore. This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc
This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc If you like what we do, please don't hestitate and subscribe to our
If you like what we do, please don't hestitate and subscribe to our