Expansion into Prescribing at the VA
Pharmacy Team Moves into Exciting New Areas of Patient Care

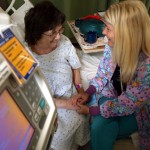
Lauren Rass, Pharm.D., a PGY1 pharmacy resident, (center left) and Lynsey Neighbors, Pharm.D., BPCS, RPD, counsel a patient.
A KEY ELEMENT of advancing pharmacy practice—and a recommendation of ASHP’s Pharmacy Practice Model Initiative—is the expansion of pharmacists’ duties to include writing medication orders.
At the Central Alabama Veterans Health Care System (CAVHCS), which serves more than 134,000 veterans in a 43-county area of Georgia and Alabama, the clinical pharmacy team has achieved this goal through a 10-year evolution.
What began with protocol-driven care in anticoagulation management has expanded into broad scopes of practice across a range of diseases and conditions. Pharmacy practice at CAVHCS now includes not only medication management, but prescribing privileges, in person and on the telephone.
Finding a Physician Champion
Expanding pharmacy practice in a health system requires strategy. When a system-wide evaluation revealed that CAVHCS wasn’t meeting its goals for lipid management, pharmacists saw an opportunity to showcase both their training and their clinical competency.
“We thought lipid management would be fairly easy to sell to management because it’s less risky than other practice areas,” said Addison Ragan, Pharm.D., BCPS, GCP, clinical pharmacy program manager. In 2002, the system opened a lipid management clinic where pharmacists had prescribing privileges under a protocol, and it wasn’t long before physicians throughout the system took notice.
“The primary care providers loved it, and they referred patients to us across the hospital setting,” said Ragan.
The following year, pharmacists moved into managing dyslipidemia in diabetes, again, under protocols. After the VA’s national clinical pharmacy leadership released guidance on dyslipidemia and diabetes and field guidance advocating broad scopes of practice, CAVHCS pharmacists worked closely with endocrinologist Neil E. Schaffner, M.D., meeting with him weekly for a roundtable discussion. The rapport that the team developed with Schaffner would later prompt him to become a physician champion for pharmacist-provided care.
Lynsey J. Neighbors, Pharm.D., BCPS, trained with Dr. Schaffner.
“He was somewhat skeptical of pharmacists stepping into this role at first, but after working with other pharmacists and later myself, he realized what pharmacists could do,” she said.
Accountability Counts
Ragan knew that if CAVHCS pharmacists wanted to work under broad scopes of practice, they would have to demonstrate their competency in quantifiable ways. The team developed competency checklists and professional practice evaluations to determine pharmacists’ knowledge and ability. She also implemented a mentoring process to improve performance as necessary. Under this system, pharmacists evaluate their peers every quarter.
“Having an accountability system in place shows leadership that you are monitoring the clinical competency of your staff,” said Ragan. “Even if there are cases where there need to be improvements, leadership can see that you are doing your due diligence.”
Such accountability helps pharmacists be their own best advocates, she added. “We become more conscientious in our documentation because we know it will be reviewed.”
When the time came to ask for expanded scopes of practice for several pharmacists, Ragan presented the evaluations to the administration, and Schaffner wrote a letter attesting to the pharmacists’ clinical competency.
With such evidence before them, the administration saw fit to grant Ragan’s request. Now, pharmacists have expanded scopes of care that allow them to prescribe and manage medications for anticoagulation, diabetes, dyslipidemia, hypertension, pain, hypothyroidism, osteoporosis, and gout, with more opportunities on the way as Neighbors dives into the world of hepatitis C management.
Saving Time and Money
Expanded scopes of care and increased pharmacist involvement in direct patient care have been time-savers for physicians and patients alike.
“Pharmacists now titrate insulin, do follow-up, work with insulin pump patients, and handle the day-to-day management of diabetes that doesn’t always fit into a physician’s schedule,” Neighbors said. She is currently training other pharmacists to take on these new roles in diabetes care.
Other pharmacists are currently handling aftercare for heart failure patients. The pharmacists meet the patients in shared appointments with cardiologists. From there, the pharmacists follow up via telephone to discuss medications, blood pressure, and post-discharge care.
Pharmacists with this expanded scope of practice have prescribing privileges that allow them to adjust medications based on the cardiologists’ goals for treatment, particularly with respect to diuretics.
“We’re hoping that, by having pharmacists engaged in diuretic management, we will be able to prevent readmissions,” Ragan said.
Pharmacist follow-up via telephone has been a boon to patients, many of whom live in rural areas and must travel as far as 80 miles to come to one of the system’s facilities. Patients aren’t charged for the pharmacists’ telephone calls, so the saved time translates into saved money, as well—enough so that the team is now testing a video telehealth program.
But beyond that, it’s just plain easier on the patients, said Ragan. “Often they’re not feeling well, so it’s taxing for them to travel long distances for simple changes in their medications.”
Pharmacy practice continues to expand at CAVHCS, Ragan added.
“Current scopes of practice are written to be very general and broad, and we can jump into managing disease states that we wouldn’t have been able to before without completely rewriting their scopes.”







 If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article.
If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article. Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore.
Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore. This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc
This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc If you like what we do, please don't hestitate and subscribe to our
If you like what we do, please don't hestitate and subscribe to our