
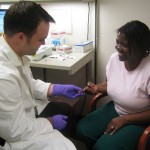
From left, Eugene Varoz, clinical pharmacist, consults with Peggy Reap, R.N., and Madhuri Segireddy, M.D., ID specialist at Chandler Regional Medical Center.
AN AGGRESSIVE ANTIMICROBIAL stewardship program established jointly by Mercy Gilbert and Chandler Regional Medical Centers led to a significant decline in unnecessary antibiotic therapy and a 25 percent reduction in costs for frequently used and expensive antibiotics. Gilbert and Chandler are two Phoenix, Ariz., hospitals in the Dignity Health network.
“Our antibiotic costs were increasing rapidly and had become one of the top drug expenditures in the pharmacy,” said Bina Patel, Pharm.D., pharmacy manager at Chandler Regional, who Patel co-led the cross-site team with Jennifer Ng, Pharm.D., former clinical pharmacy supervisor at Mercy Gilbert.
Dr. Patel noted that just five antibiotics were responsible for 60 to 70 percent of antibiotic costs at the two facilities. “We also found that these broad-spectrum antibiotics were often prescribed inappropriately,” she said.
Neither hospital’s pharmacy regularly reviewed antibiotic order patterns, resulting in inconsistent prescribing practices and antibiotic overuse.
The hospitals formed a multidisciplinary team tasked with creating an antimicrobial stewardship program that could be incorporated into routine medication management. In addition to Drs. Patel and Ng, the team included an infectious disease pharmacist, an infection preventionist, a microbiologist, an infectious disease physician, an emergency medicine physician, and a hospitalist.
Identifying Underlying Causes of the Problem
Using a form of Lean methodology called Transformational Care (TC), the team set out to identify the root causes of the problem and create quick and efficient solutions. TC and Lean methodology help to streamline and simplify systems and eliminate waste. Each team member underwent 12 weeks of TC training.
The team discovered that pharmacists were playing only a limited role in managing infectious disease therapies. Standardized diagnostic order sets, pharmacy reviews, and interventions also were lacking.
In the face of these challenges, the team developed criteria for using broad-spectrum, high-cost antibiotics and formulated evidence-based guidelines for antibiotic use. They also created an antibiogram displaying the sensitivities of various isolated bacterial strains to different antibiotics.
This information was then published in pocket guides and distributed to prescribers. Standardized adult antibiotic order sets based on frequent diagnoses (e.g., pneumonia, cellulitis, and urinary tract infections) were also developed to improve the accuracy of antibiotic selection.
“The forms are targeted primarily at hospitalists and emergency department physicians so they don’t have to spend time thinking about what they need to do empirically,” explained Dr. Patel. “The physicians can use the form to simply check off the correct antibiotic based on the diagnosis and send it to the pharmacy. Because the drug choice was selected from the approved form, the order doesn’t need to be reviewed.”
For inpatients, an infectious disease pharmacist reviews orders for the top five targeted antibiotics to ensure that they are well matched to an empiric diagnosis. When culture results become available, the pharmacist rechecks to determine if the therapy is appropriate. If a change is needed, the pharmacist calls the prescribing physician to recommend a more suitable antibiotic, decrease the dose, switch from IV administration to an oral form, or discontinue therapy entirely.
Physician Education and Metrics
The program has been a great success. During its first year, pharmacists conducted 1,966 interventions at both hospitals, 93 percent of which were accepted by physicians.
“We also conducted physician education to increase awareness of antimicrobial stewardship and what it means to the quality of patient care,” said Dr. Patel. “That helped to win acceptance.”
To gauge the impact of the initiative, the team tracked, among other metrics, the average daily defined doses (DDD) of the five target antibiotics, the number of patients prescribed the target drugs, the length of therapy, and drug costs.
The results have been impressive. During the program’s first year, the average DDD decreased for all of the top five targeted antibiotics—in one case by more than 70 percent (see box). The cost per inpatient day for the five drugs decreased 26.4 percent, and the total antibiotic cost per inpatient day dropped 14.2 percent. The number of patients prescribed the target antibiotics for more than five days also declined.
After the first year, the changes leveled out, which Dr. Patel expected. Now, near the end of the program’s third year, the challenge is to hold onto the gains and widen the net.
“We achieved a significant reduction from baseline in both drug usage and costs. Now we need to maintain that progress,” she said. “We’ve also expanded the program to look at other antibiotics.”
Recruiting Champions
The initiative has raised the visibility of clinical pharmacists, according to Dr. Ng, now a clinical pharmacist at Banner Baywood Medical Center in Mesa, Ariz.
“Initially, some of the physicians were not used to pharmacist interventions, at least with antibiotics,” she said. “Later, their responses became far more positive, and they said they appreciated and even expected the calls. Resistance really dissipated once the doctors understood what we were trying to accomplish.”
Dr. Ng emphasized the importance of a multidisciplinary team and having a physician advocate on the team.
“Having at least one physician champion goes a long way,” she said, noting the support of an infectious disease doctor on their team. “It shows the rest of the hospital that the program is not just the pharmacy out there on its own, and it drives home the point that there’s a bigger goal in terms of patient care.”
Administrative support, another factor that was crucial to the program, was present from the start.
“The pharmacy and the infection control physicians led the way,” said Peter Menor, vice president of operations at Chandler Regional and the executive sponsor for the initiative. “My role was to give them the resources to get the job done. The program spread very quickly. Before we knew it, the entire medical staff was involved. It’s been very well received and it’s had an enormous impact on patient care.”
–By Steve Frandzel








 If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article.
If you want to contribute tutorials, news or other stuff please contact us. We pay 150 for each approved article. Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore.
Consectetur adipisicing elit. Sed do eiusmod tempor incididunt ut labore. This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc
This site uses valid HTML and CSS. All content Copyright © 2010 Newscast, Inc If you like what we do, please don't hestitate and subscribe to our
If you like what we do, please don't hestitate and subscribe to our